Irritable Bowel Syndrome (Ibs) Ensure This Is Checked and Diagnosed Correctly to Avoid Potential Serious Consequences.

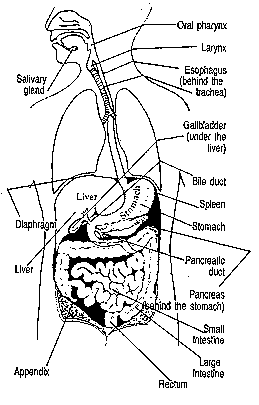


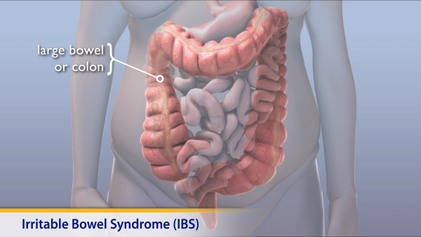

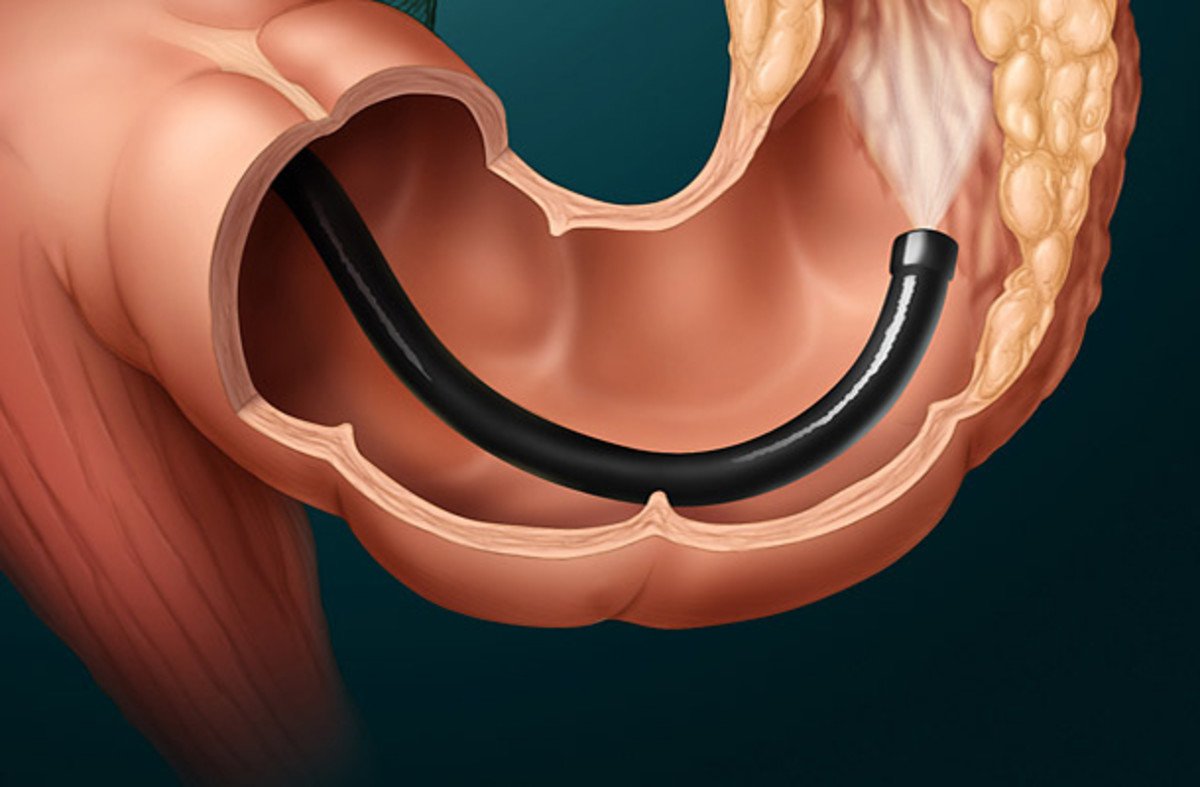
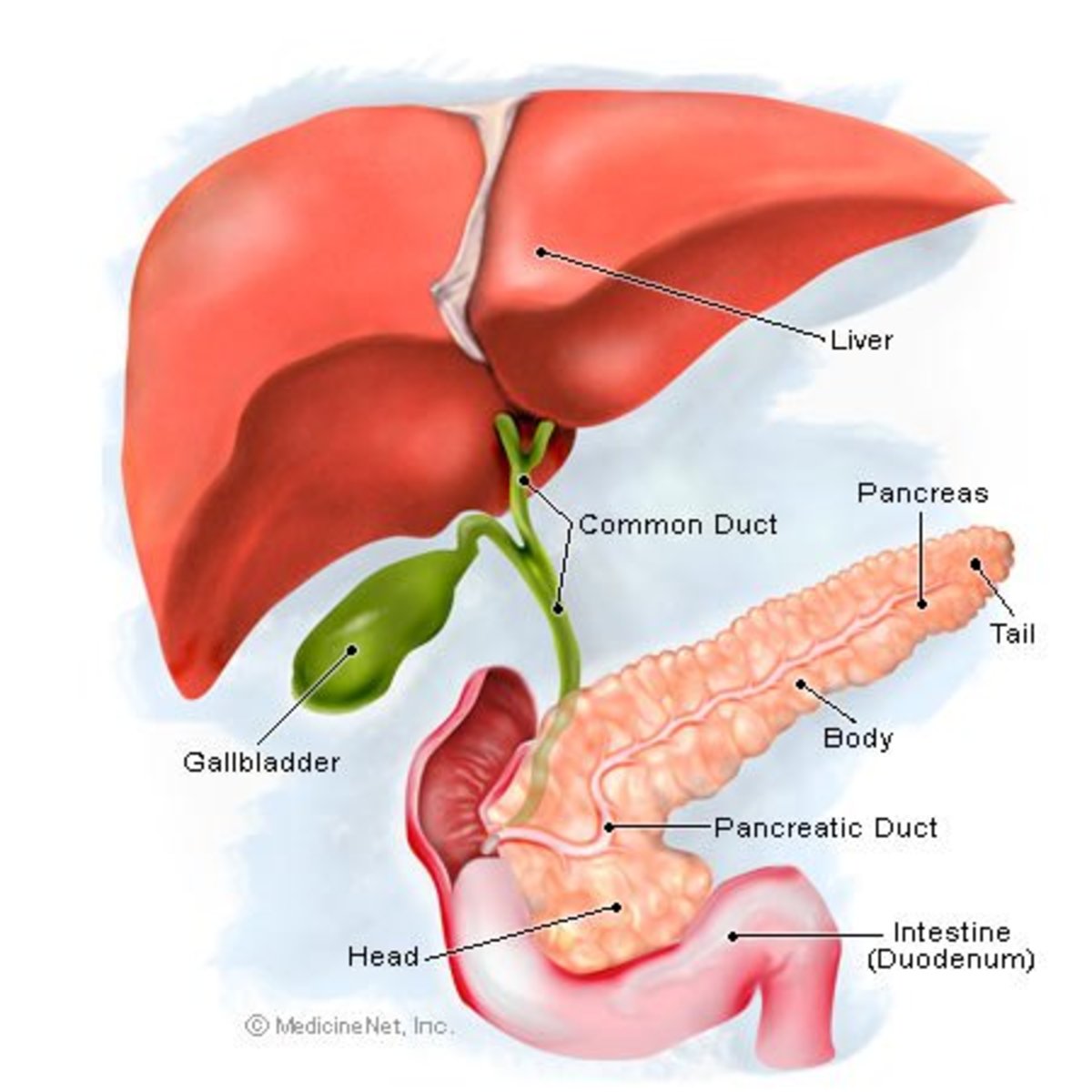
Irritable Bowel Syndrome, more commonly known as IBS or Spastic Colon has become the scourge of modern living. Many believe it is a result of a digestive system that has not evolved sufficiently to cope with processed foods, stress and pollution. IBS has no known organic cause and sufferers experience chronic abdominal pain, discomfort, bloating, and a change in their bowel movements.
The first stage in the treatment of IBS is to ensure that it is, indeed, IBS we are suffering.
With IBS the pain and discomfort that you feel may occur in varying parts of the abdomen and usually comes and goes with the duration varying greatly. You can find the pain often eases when you pass stools or wind. Bloating and swelling of your abdomen may occur from time to time and you may pass more wind than usual.
It is necessary to visually examine the bowel movement as the doctor will need to know its appearance.
Some people have bouts of diarrhoea, and some have bouts of constipation, while others will have bouts of diarrhoea that alternate with bouts of constipation.
The stools can become small and pellet-like, while in others the stools become watery or ribbon like with mucus mixed with the stools. You may feel a continued need to empty your bowels even after going to the toilet. With some you have an urgent need to get to the toilet quickly. This morning rush is common and so is an urgent need to go to the toilet several times shortly after getting up.
Being able to easily access public toilets is important if you have sudden, urgent bouts of diarrhoea. Two schemes that can help are:
The IBS Network – which provides members with a Can't Wait Card to help them gain immediate access to toilet facilities in offices, stores and other UK businesses
https://www.theibsnetwork.org/cant-wait-card/
The National Key Scheme (NKS) by Disability Rights UK – which provides access to the thousands of locked disabled toilets around the country
More general symptoms sometimes occur, including: nausea, headache, belching, poor appetite, tiredness, backache, muscle pains, feeling full quickly after eating, heartburn, and associated irritable bladder.
Many people suffer mild symptoms re-occurring frequently over a long period of time, while others can experience significant major flare-ups of symptoms within a short space of time.
Note: passing blood is not a symptom of IBS. You should tell a doctor if you pass blood. This can sometimes occur as IBS and haemorrhoids often go hand in hand and one can aggravate the other.
The symptoms of IBS are similar to many other disorders, some minor but importantly some very serious and for that reason we must be sure of our diagnosis. This is not really a case for self-diagnosis. Before assuming the problem is IBS it is vital that a reliable medical diagnosis is made (be careful doctors have a habit of dismissing such digestive disorders as IBS rather than become involved in more involved diagnosis - insist on a proper examination).
OK let’s assume we are now definitely dealing with IBS. Nobody dies from IBS but it causes much suffering, inconvenience and loss of working days. There is no current known cure only the ability to lessen or control the symptoms.
Essential oils also cannot cure IBS but it is one tool available to make life more normal and acceptable.
I am always reluctant to suggest ingesting essential oils although this is routinely done in native medications. The difference is in the purity of the essential oil we are using. Native medication uses pure extracted oils (carried out through crude simple distillation processes) or using what is known as essential waters, with no adulteration or cheap oils as additions. Oils on sale commercially are most often used as perfumes or in oil burners but for ingestion or absorption through the skin into the blood they must be therapeutic grade and this is vitally important. I will always stress this in any of the guides I publish – you must purchase the best verified quality essential oils you can afford. This does not mean the most expensive, but invariably quality often must be paid for.
Because many of you will not be familiar with Essential Water a few words may be useful. They are normally derived from the process used in the production of Essential Oils but it is important to ensure they only come from the steam distillation process with nothing added or taken away. Some Essential Waters are sold only for commercial (and this includes Chemist Shops) deodorising use or perfumes and are useless, indeed dangerous, to use therapeutically – if in doubt do not use. You may find Essential Waters difficult to source, if you have a problem try -
http://www.organic-creations.com
Really the only oil to ingest is Peppermint – either the essential oil or essential water. This has a good track record for centuries in the treatment of IBS. Peppermint essential oil – one drop mixed into one dessert spoon (15ml) Manuka runny Honey (Do NOT exceed this dose – Peppermint Essential Oil is listed as GRAS (generally regarded as safe) and a LD50 fatal dose in a 70kg (155 pounds) human is 330ml (about the size of a can of Coke), which is a huge amount). Nevertheless essential oils by their very nature are highly concentrated and overdoses can cause internal irritation and possible burning of the throat. In addition ingestion under any circumstances is not suitable for those with heartburn or active gastric ulcers. If you are at all doubtful please consult either your doctor or local aromatherapist first, where you can discuss your particular medical history.
Peppermint essential water – 5ml into a medium glass of fruit juice or tea 3 times a day. The same warnings as above apply.
The decision to ingest Peppermint Essential Oil or Water must be yours. Without access to your medical history or any examinations or diagnosis that has been made by a medical practitioner, I am not in a position to recommend or otherwise.
If you are at all concerned about ingesting Peppermint then very good results have been achieved by massaging the abdomen with the following essential oils in an Argan Oil preparation.
For calming effect use Roman Chamomile and Lavender
Together with Anise, Peppermint, Ylang Ylang and Rose
Clary sage and Melissa can be useful additions but NOT if pregnant.
Please remember the above oils are for external application in a carrier oil only and must NOT be ingested (swallowed)
As I said at the start there is no one product that will cure IBS or even remove the symptoms, rather it is a combination of different approaches that can offer the best relief.
Your diet should contain a good balance of proteins and fats and it would be advantageous to include a good multivitamin but ensure you take 2 x 150mg of Magnesium and an Omega-3 capsules (1000mg) preferably Flaxseed (which has a good effect on IBS) rather than Fish Oil. In addition you should also consider adding digestive enzyme supplements and probiotics and a selection of these should be available at your health food store.
A traditional herbal remedy is inulin (not insulin) which is contained in Dandelion (taraxacum) root (be certain it is the root not the leaf). It is the food of the gut bacteria and thereby aids digestion. In trials it increased the levels of lactobacillus bifido bacteria and decreased the pathogenic flora responsible for IBS. Take 250-500mg three times daily.
For years it has been suggested that high fibre diets can bring about relief from IBS, however more recent research has shown that it’s the type of fibre that is important. There are two sources, soluble and insoluble fibre.
Dietary sources of soluble fibre include oats, ispaghula (psyllium), nuts and seeds, some fruit including bananas and apples and root vegetables such as, carrots and potatoes pectins, barley, rye and golden linseeds. A fibre supplement called ispaghula powder has been found to be the most beneficial and is available from health food shops
Insoluble fibre is chiefly found in corn (maize) bran, wheat bran, cereals, wholegrain bread and some fruit and vegetables. Despite the advertisements in particular, avoid bran as a fibre supplement. If you have diarrhoea, you may find it helps to cut down on the insoluble fibre you eat. It may also help to avoid the skin, pith and pips from fruit and vegetables. Therefore be careful in using such devices as Nutri Bullet which will liquidise the whole fruit or vegetable.
There is a new supplement available based on fennel, peppermint and cardamom oils which will sooth the mucous membranes.
L-glutamine will help to repair the intestinal tissues that have become damaged.
For all digestive disorders you should start the day with a quarter of a glass of aloe vera juice (flavoured ones are available) with the same again before bed.
Slippery Elm is thought to calm irritation in the intestinal system. I have no proven trials information to support this.
Amalaki and Triphala are Ayurvedic herbal preparations thought to reduce abdominal pain and bloating. Again I have no trials information to support this.
Properly diagnosed IBS is often severely aggravated by stress and you should not dismiss a few sessions with an accredited Reiki practitioner, who have been shown to achieve remarkable results with both humans and animals. (I mention animals only because you can’t fool animals – they have no expectation and it either works or doesn’t !)
Other relaxation techniques include meditation or breathing exercises
Physical activities – such as yoga, Pilates or tai chi
If you are particularly stressed, you may benefit from a talking therapy, such as stress counselling or cognitive behavioural therapy (CBT).
Exercise: Many people find that exercise helps to relieve the symptoms of IBS. Your GP can advise you on the type of exercise that is suitable for you. Aim to do a minimum of 150 minutes of moderate-intensity aerobic activity, such as cycling or fast walking, every week. The exercise should be strenuous enough to increase your heart and breathing rates.
Medication: A number of different medications can be used to help treat IBS, including:
antispasmodics – which help reduce abdominal (stomach) pain and cramping Antispasmodics work by helping to relax the muscles in your digestive system. Examples of antispasmodic medicines include mebeverine and therapeutic peppermint oil. Side effects associated with antispasmodics are rare, however, people taking peppermint oil may have occasional heartburn and irritation on the skin around their bottom.
laxatives – which can help relieve constipation Bulk-forming laxatives are usually recommended for people with IBS-related constipation. They make your stools softer, which means they are easier to pass. It's important to drink plenty of fluids while using a bulk-forming laxative. This will help prevent the laxative from causing an obstruction in your digestive system. Start on a low dose and then, if necessary, increase it every few days until one or two soft stools are produced every one or two days. Do not take a bulk-forming laxative just before you go to bed. Side effects associated with taking laxatives can include bloating and wind. However, if you increase your dose gradually, you should have few, if any, side effects.
antimotility medicines – which can help relieve diarrhoea The antimotility medicine loperamide is usually recommended for IBS-related diarrhoea. Loperamide works by slowing contractions of muscles in the bowel, which slows down the speed at which food passes through your digestive system. This allows more time for your stools to harden and solidify. Side effects of loperamide can include stomach cramps and bloating, dizziness, drowsiness and rashes.
low-dose antidepressants – These were originally designed to treat depression, but can also help reduce stomach pain and cramping independent of any antidepressant effect Two types of antidepressants are used to treat IBS – tricyclic antidepressants (TCAs) and selective serotonin reuptake inhibitors (SSRIs). TCAs, such as amitriptyline, are usually recommended when antispasmodic medicines have not been able to control the symptoms of pain and cramping. They work by preventing signals being sent to and from the nerves in your digestive system. However, TCAs will only start to provide relief after three to four weeks, as your body gets used to the medication. Side effects of TCAs can include a dry mouth, constipation, blurred vision and drowsiness. These side effects should improve within a few days of starting the medication. Tell your GP if the side effects become a problem – they may prescribe another type of antidepressant. SSRIs are an alternative type of antidepressant. Examples of SSRIs that are used to treat IBS include citalopram, fluoxetine and paroxetine. Common side effects of SSRIs include blurred vision, dizziness and diarrhoea or constipation.
If you experience persistent or frequent bloating, Kings College London has developed a special diet called the low FODMAP diet which has been found to be effective.
FODMAP stands for fermentable oligosaccharides, disaccharides, monosaccharides and polyols. These are types of carbohydrates that aren’t easily broken down and absorbed by the gut. The effect of this means they start to ferment in the gut relatively quickly, and the gases released during this process can lead to excess wind and bloating.
A low FODMAP diet involves restricting your intake of certain foods that are high in FODMAPs, such as some fruits and vegetables, animal milk, wheat products and beans.
If you want to try the low FODMAP diet, it’s best to do so under the guidance of a professional dietitian, who can ensure your diet is still healthy and balanced. You can ask your GP or specialist to refer you.
You can read more about the low FODMAP diet on the Kings College London website. http://www.kcl.ac.uk/lsm/research/divisions/dns/projects/fodmaps/index.aspx
All formulations are given for guidance only. If you suffer any adverse reactions you must discontinue the treatment immediately and seek medical advice if necessary
Have you ever suffered from IBS and was it diagnosed medically ?
© 2012 Peter Geekie